INTRODUCTION
Dengue is among the most important arboviral infections affecting humans and has emerged as one of the most significant public health concerns worldwide, primarily in tropical and subtropical regions (1,2, 3, 4, 5). The causative agent of the infection is Dengue virus (DENV), an RNA virus (single-stranded, positive-sense) belonging to the genus Flavivirus in the family Flaviviridae (1). Four antigenically different serotypes of the DENV (i.e., DENV-1, DENV-2, DENV-3, and DENV-4) are responsible for causing anything from a mild fever to the life‐threatening dengue hemorrhagic fever (DHF) or dengue shock syndrome (DSS) (1, 2, 5, 6, 7). The virus is transmitted by female anthropophillic Aedes mosquitoes, most commonly Ae. aegypti and less commonly Ae. Albopictus(2, 8).
The global burden of dengue has increased significantly in the last two decades. According to a recent report by the World Health Organization (WHO), dengue has become endemic in more than 100 countries, with an estimated 100–400 million infections occurring each year (4, 9). Roughly 3.9 billion people, i.e., about half of the world population, are at risk of dengue infection. The burden of dengue is notably concentrated in tropical and subtropical areas, particularly in South East Asia and South Asia, where 70% of cases occur (4).
Bangladesh, situated in South Asia with a population of 165 million and nestled within the tropical belt, has been vulnerable to various disease outbreaks. High population density, climate change, and inadequate health facilities are some of the contributing factors to the high outbreak susceptibility of the country. Cholera, for example, has been historically associated with the region and is still a significant public health threat. In 2022, Bangladesh experienced a severe cholera outbreak, with the icddr,b (International Centre for Diarrhoeal Disease Research, Bangladesh) Dhaka Hospital handling over 1300 patients and approximately 42,000 cases of diarrhea between March 1 and April 10, 2022 (10).
The COVID-19 pandemic, which reportedly entered Bangladesh on March 8, 2020, has had a significant impact on the country, resulting in 2,049,985 cases and 29,494 deaths (as of May 12, 2024) (11). As the COVID-19 pandemic has overwhelmed the healthcare system, managing other diseases such as dengue has become more challenging (4). Dengue and other vector-borne diseases such as malaria, and chikungunya are becoming more common in Bangladesh, particularly due to changing climate conditions (12). The rise of dengue cases in recent years has exacerbated the public health situation in the country. The geographic location of Bangladesh, characterized by warm and humid climates, as well as climate change provides an ideal breeding ground for the spread of DENV. Moreover, globalization, increased travel, and rapid unplanned urbanization have amplified the risk of dengue transmission (1, 4, 13, 14).
Environmental factors such as warm temperature, humidity, and rainfall are positively correlated with dengue transmission (15, 16, 17). Alarmingly, the breeding environment for the Aedes mosquitoes has become more favorable due to the increased amount of rainfall, and rise in temperature and humidity due to climate change (12). Consequently, the dengue outbreaks in recent years have been unprecedentedly severe in Bangladesh. In addition, Bangladesh is consistently at risk of importing new dengue strains due to its proximity to countries where dengue is endemic (12, 18). Introducing a new serotype has been responsible for the deadlier secondary dengue infection possibly due to antibody-dependent enhancement (ADE) (19, 20).
Bangladesh has faced recurring dengue epidemics since 2000 (18). However, dengue has become a serious public health burden, particularly during the last 6 years, with both cases and deaths increasing significantly. After a record-breaking outbreak in 2018 and 2019, the reported cases declined during COVID-19 lockdown. However, the cases have again escalated unprecedentedly and surpassed all previous outbreaks in 2022 and 2023. Climate change and the emergence of various dengue virus serotypes are considered responsible for recent severe dengue outbreaks. Furthermore, the country appears to be unprepared to manage dengue, as the government’s dengue management policy has been criticized as inadequate, which further exacerbated the dengue situation.
GLOBAL OCCURRENCE OF DENGUE
The global spread of dengue can be attributed to World War II (1939-1945), which brought significant ecological, demographic, and epidemiologic changes, leading to increased transmission of the virus. After World War II, dengue became a public health burden in Southeast Asia particularly due to the rapid urbanization. Dengue was not a public health threat in the Americas, Africa, and Oceania for two decades after World War II largely due to Ae. aegypti eradication efforts initiated by the Pan American Health Organization (PAHO) in the Americas. However, the discontinuation of these efforts in the early 1970s led to the gradual reinfestation of the region by Ae. aegypti, paving the way for the resurgence of dengue (21).
The dengue burden has been exacerbating globally over the past 30 years. From 1990 to 2019, the number of dengue incident cases has been estimated to increase by 85.5% (22). Between 2000 and 2019, a tenfold surge in reported dengue cases worldwide was documented by the WHO, increasing from 500,000 to 5.2 million. In 2019, an unprecedented peak was marked, with reported instances spreading across 129 countries (23).
The Americas reported over 4.1 million cases in 2023 (as of 11 December), accounting for approximately 80% of all cases. Brazil, Peru, and Mexico were the most affected countries in the Americas, with 2,909,404; 271,279; and 235,616 reported cases, respectively (as of 12 November) (23).
In Africa, outbreaks were reported in 15 out of 47 countries, notably in Burkina Faso with 146,878 cases (As of 18 December). The Western Pacific region reported over 500,000 cases, with the Philippines (167,355) and Vietnam (149,557) among the most affected (as of 7 December) (23).
In 2023, Southeast Asia witnessed a significant increase in dengue cases, with Bangladesh reporting 308,167 cases and 1,598 deaths, and Thailand reporting 136,655 cases and 147 deaths ((as of 22 November). Remarkably, Bangladesh reported more dengue cases (308,167) than the entire WHO Region of Africa (171,991) in 2023. The number of dengue-related deaths in Bangladesh (1,598) surpassed both the WHO Western Pacific Region (750) and the WHO Region of Africa (753) in the year (23).
FROM SPORADIC TO EPIDEMIC: THE CHANGING TREND OF DENGUE OUTBREAKS IN BANGLADESH
Dengue outbreaks became a noticeable public health burden in Southeast Asian countries after World War II, principally due to urbanization (14, 18, 21, 24).
In 1964, dengue was first recorded in Bangladesh (then East Pakistan) and was known as “Dacca fever” (25). From 1964 to 1999, Bangladesh experienced sporadic transmission of the dengue virus (Table 1). During this period, dengue cases were not officially reported or clinically diagnosed but serological evidence for the presence of dengue was found in serosurveillance studies among febrile patients (26, 27, 28). Thus, dengue might have already established a significant presence in the country before the 21st century, but escaping clinical attention due to the lack of suitable laboratory facilities and the nonspecific nature of dengue’s clinical characteristics.
Table 1.
Three phases of dengue in Bangladesh
| Timeline | Type of transmission | Cases | Deaths | Prevalent serotypes | References |
|---|---|---|---|---|---|
| 1964-1999 | Sporadic | Not reported | Not reported | Unknown | (18, 39) |
| 2000-2017 | Epidemic | 40,476 | 268 |
DENV-3 (2000-2002) DENV-1 and DENV-2 (2013-2017) | (18, 27, 31.32, 43) |
| 2018-2023 | Epidemic | 524,629 | 2,282 |
DENV-1 and DENV-2 (2018) DENV-3 (2019-2022) DENV-2 (2023) | (12, 31, 32, 36, 39) |
The first official outbreak of dengue occurred in Bangladesh in 2000, with 5551 cases and 93 deaths reported. Dengue hemorrhagic fever was also reported for the first time in that year (18, 29, 30). Since then, several outbreaks have been observed throughout the decade. During the dengue outbreaks from 2000–2017, a total of 40,476 cases and 268 deaths have been reported with two major peaks in 2002 (6,232 cases) and 2016 (6,060 cases) (31).
The dengue situation in Bangladesh has worsened in recent years, with an unprecedented increase in cases and fatalities. In 2018, a record-breaking 10,148 dengue cases with 28 deaths were reported which is about 25% of all the previous cases reported i.e., 2000-2017 (Fig. 1). In 2019, the country faced another severe dengue outbreak with 101,354 cases and 164 fatalities, exceeding the total number of reported cases of all previous years (2000-2018) by about 200%. In 2020 and 2021, the country saw a decline in the number of dengue cases, with 1,405 and 28,429 cases, respectively (32). This decline, especially in 2020, may be attributed to the COVID-19 related lockdown resulting in the disruption of construction works which otherwise provide a breeding environment for dengue-carrying mosquitoes (33). A strong association between COVID-19-related societal disruption and reduced dengue incidence has been found across many dengue-endemic regions (34). The underreporting and misdiagnosis of dengue during the efforts to manage the COVID-19 crisis could also contribute to the misleadingly low cases in Bangladesh (35).
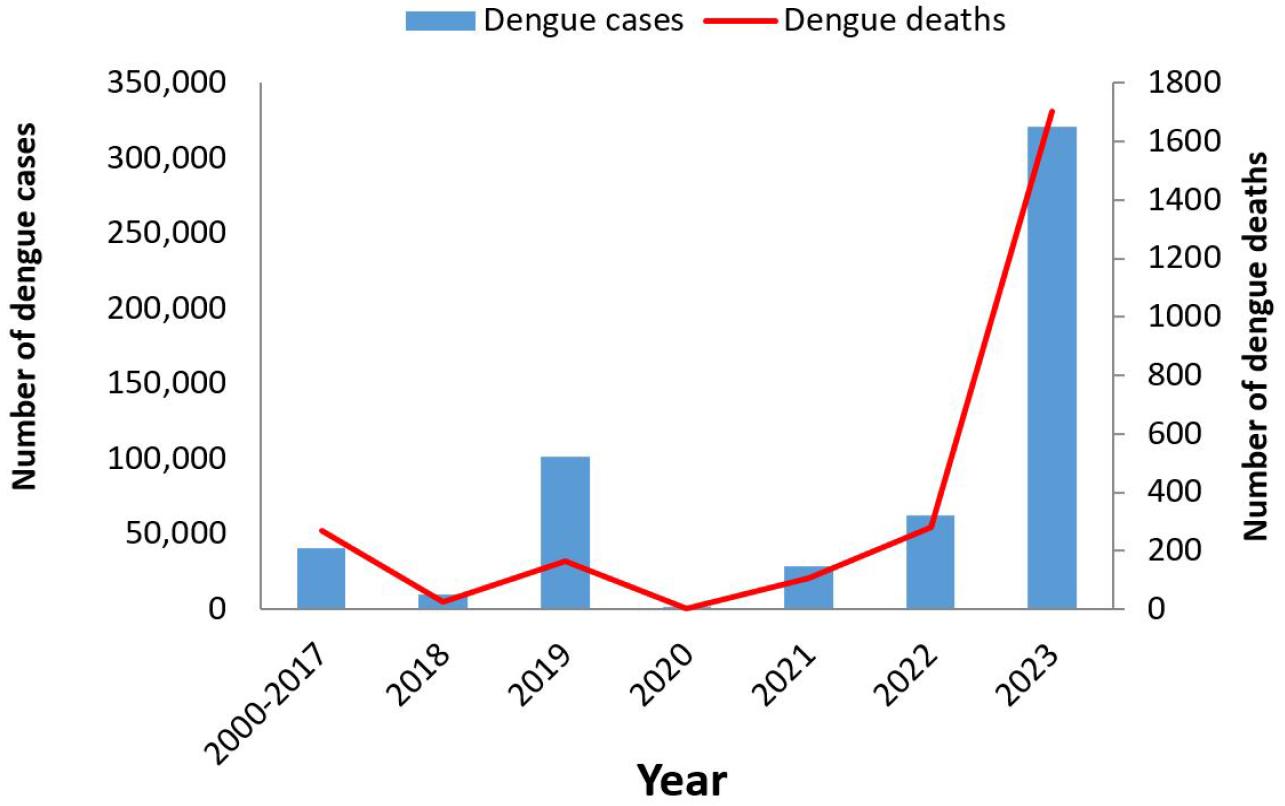
Fig. 1
Reported dengue cases and deaths by years where bar and line indicate dengue cases and dengue deaths, respectively. Here, the Y axis and Y’1 axis represent the number of dengue cases and the number of dengue deaths, respectively in different years/year ranges in the X axis. Since 2018, the cases have increased dramatically. Cases in 2019, 2022, and 2023 were higher than the combined cases of 2000-2017 (23, 27).
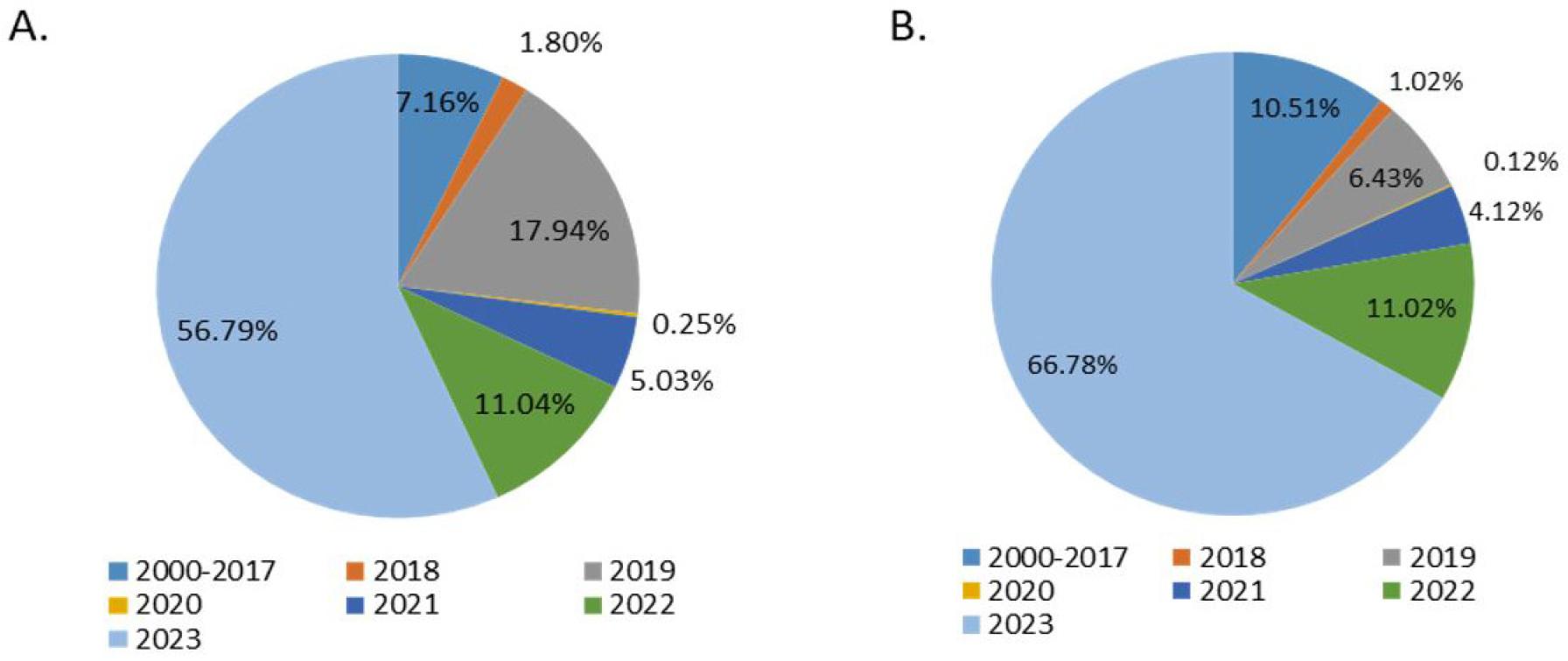
In 2022, the incidence of dengue again surged to the second-highest level, accompanied by 61,732 cases, and 281 deaths (33, 34, 35). The surge in dengue infections during 2023 has surpassed all the previous outbreaks, with a reported total of 61,732 cases and 281 deaths, marking the deadliest year in the nation’s history (35-36). The dengue cases in this single year contribute to nearly 57% of the total dengue cases (Fig. 2A) and 67% of total dengue deaths (Fig. 2B) recorded from 2000 to the present.
SEASONAL EXTENSION OF DENGUE OUTBREAK
Dengue cases usually follow a seasonal pattern as it coincides with rainfall. The increased rainfall during rainy seasons creates ideal conditions for the accumulation of stagnant water in artificial containers (e.g., old tires, bottles, pots, broken appliances, plastic containers) providing breeding grounds for the Aedes mosquito, the vector for transmitting the disease (37).
Bangladesh receives a major portion of annual rainfall during the summer monsoon (also known as southwest monsoon) season (June–September). The summer monsoon makes up approximately 72% of Bangladesh’s total annual rainfall (38).
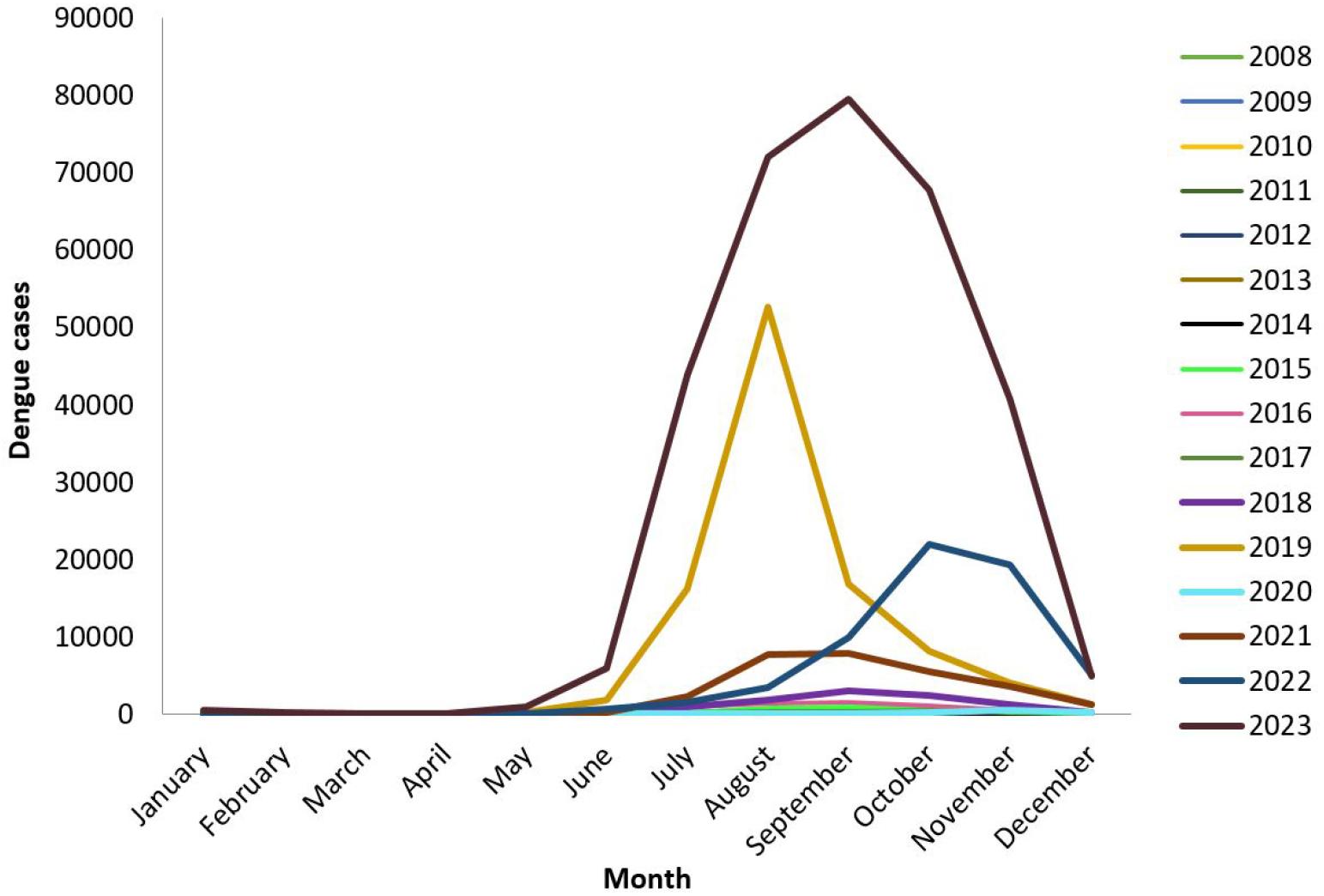
Until recent years, dengue cases usually started from July and ended in October. However, this seasonal pattern has been observed to be shifted as the cases appeared to rise much earlier than expected. In 2023, there were already over 900 cases in May and the peak month of dengue cases was September (with 79,598 cases) (Fig. 3). In comparison, the peak month in the previous year (2022) was October (with 21,932 cases). During the 2019 outbreak, the peak incidence occurred in August, with over 50% of all cases reported during that month (39).
Bangladesh’s climate conditions are becoming more favorable for the transmission of dengue due to excessive rainfall, waterlogging, flooding, rise in temperature and humidity, and the unusual shifts in the country’s traditional seasons. According to a pre-monsoon Aedes survey, the density of mosquitoes, and the number of potential hotspots has reached their highest levels in the last five years (12). Consequently, the dengue outbreaks in recent years are unusual in terms of seasonality, with cases reported throughout the year. The pre-monsoon (January-April) cases were negligibly low until 2012 (Table 2, Fig. 4A). However, pre-monsoon, as well as post-monsoon (September-December) cases began emerging in 2013 and became significantly high in 2023. Remarkably, cases in winter, which is quite unusual considering the supposedly low temperature and rainfall in the season, have reached an alarmingly high level in 2023 with over 50% of cases in the cold season occurring this year (Fig. 4B). This extension of dengue was predicted in a 2021 study which projected that the seasonality of the dengue transmission season may diminish at the end of 21st century under the consistently changing climate of Bangladesh and eventually become an all-year-round phenomenon, causing outbreaks at any point in time (40).
Table 2.
Seasonality of dengue. Pre-monsoon cases in recent years have increased significantly
| Seasons | Months | Dengue cases | References | ||
|---|---|---|---|---|---|
| 2000-2012 | 2013-2017 | 2018-2023 | |||
| Pre-Monsoon | January-April | 4 | 381 | 1,685 | (31, 32, 36) |
| Monsoon | May-August | 14,546 | 5,460 | 213,183 | |
| Post-Monsoon | September-December | 11,822 | 8,274 | 309,761 | |
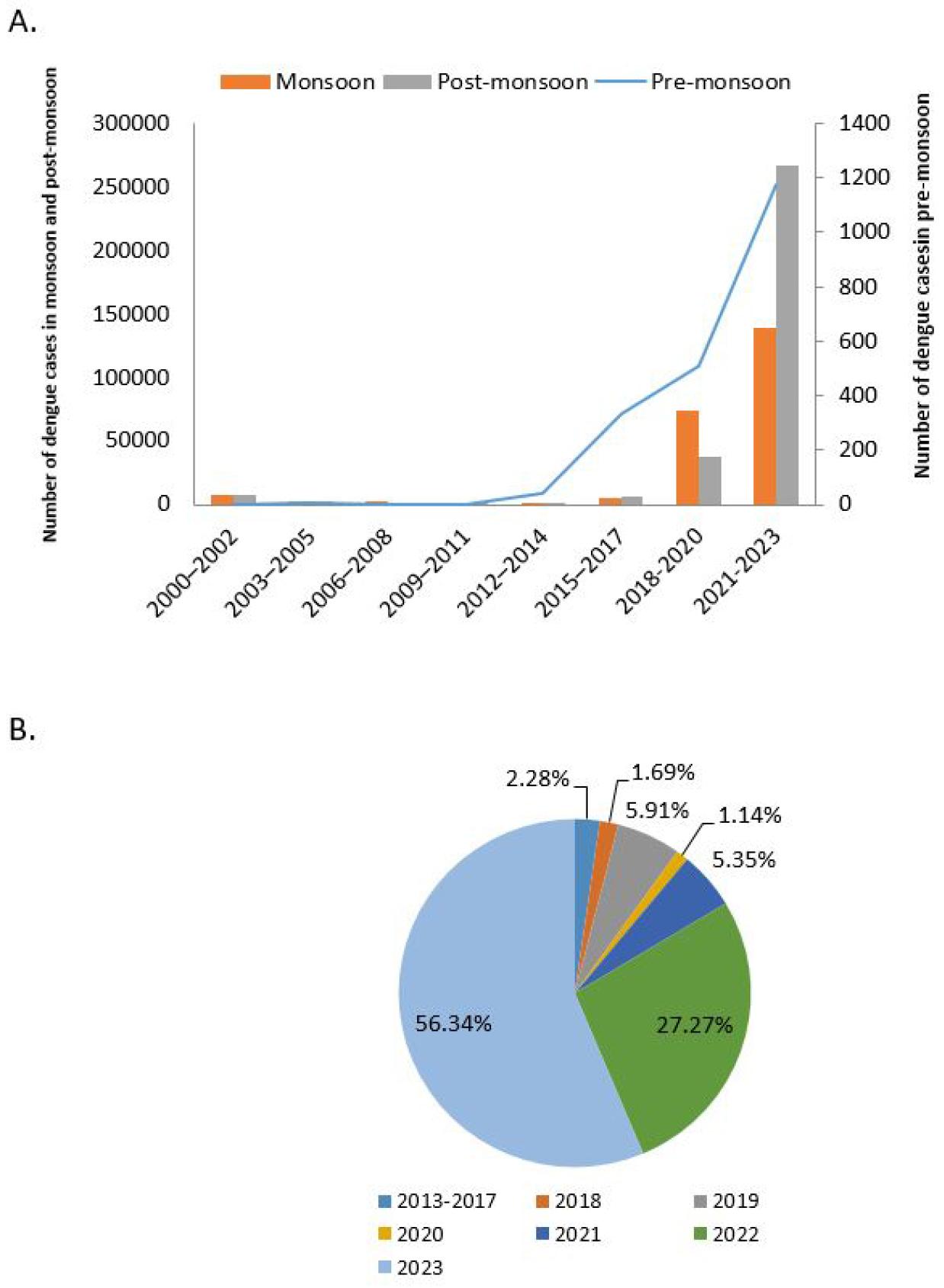
Fig. 4
(A) Seasonal pattern of dengue outbreaks in the last 23 years. The Y denotes the number of dengue cases in monsoon and post-monsoon, whereas the Y’1 axis denotes the number of pre-monsoon cases. Besides the orange bar, the ash bar, and line indicate monsoon, post-monsoon, and pre-monsoon, respectively. Pre-monsoon cases started to appear in 2013 and reached an all-time high in 2023 (22, 23, 27). (B) Distribution of winter (November, December, January, and February) cases by year. About 83% of all winter cases have occurred in the last two years (2022 & 2023) (23, 27).
During the last 8 years (2016-2023), there has not been a single dengue-free month (Fig. 5A), and months with over 100 cases has been increased. In 2023, at least 100 cases were reported in all 12 months (Fig. 5B).
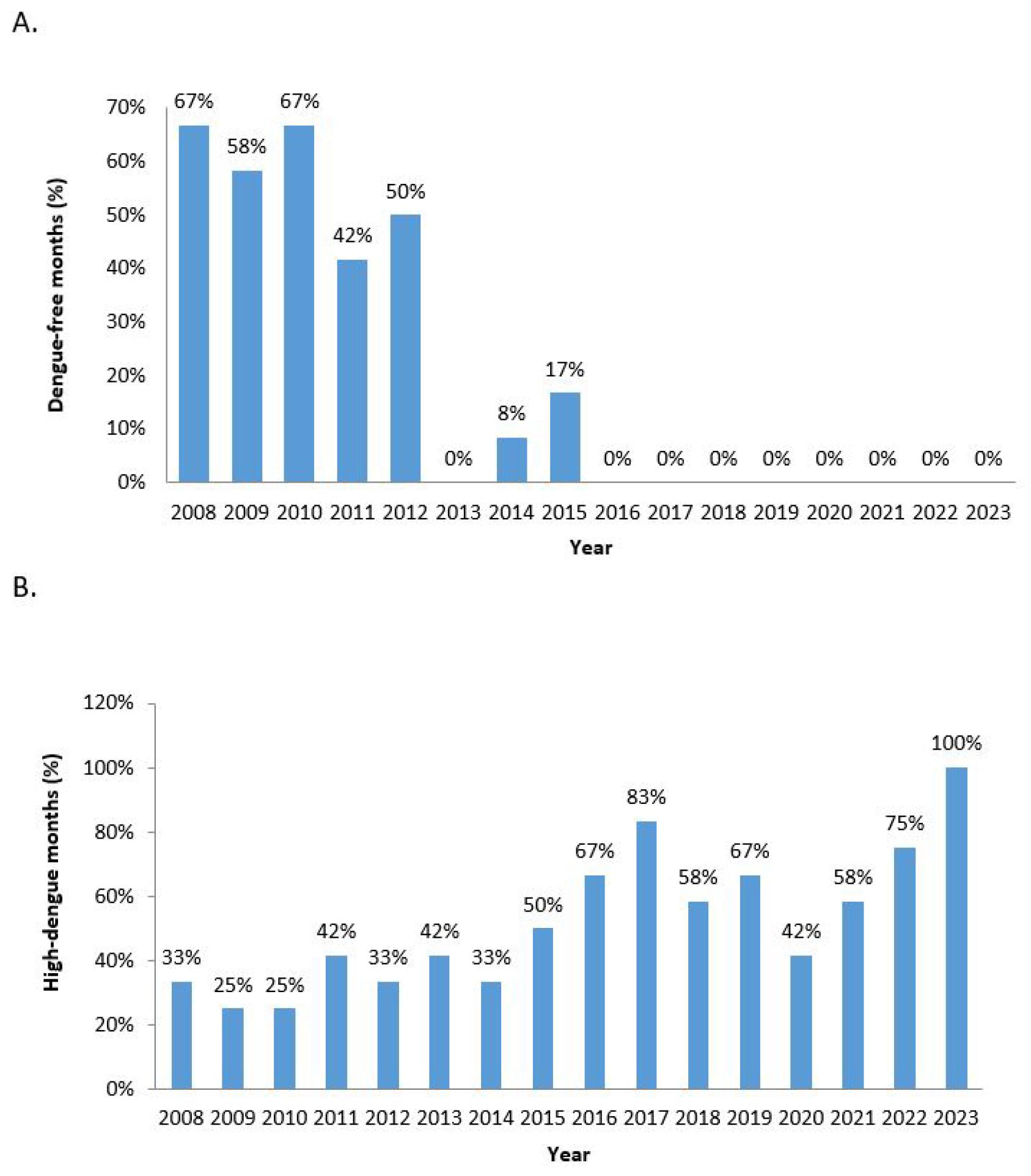
Fig. 5
(A) Percentage of dengue-free months (2008-2023). Until 2012, most months particularly in the winter season, were free from dengue. However, seasonality has started to extend from 2013 and there has not been a single dengue-free month in the last 8 years (2016-2023). (B) Percentages of high-dengue (>100 cases) months (2008-2023). All months in 2023 had received more than 100 cases (23, 27).
SEROEPIDEMIOLOGICAL PATTERN
Dengue fever results from infection with 4 serotypically distinct dengue viruses, i.e., DENV-1, DENV-2, DENV-3, and DENV-4. These 4 serotypes are characterized by antigenic differences, resulting in varied interactions with Dengue-specific antibodies found in human blood serum. The genetic diversity is much more complex as multiple genotypes exist within each serotype. A 30–35% diversity in amino acids has been found to exist among the serotypes. (41). Due to the antigenic variation, infection with 1 serotype provides immunity against that specific serotype but does not confer immunity against the other 3 serotypes (12). Secondary infections with a different serotype can lead to a severe form of dengue, i.e., dengue hemorrhagic fever (DHF) or dengue shock syndrome (DSS). This phenomenon has been attributed to antibody-dependent enhancement (ADE) which occurs when preexisting antibodies from a primary DENV infection bind to a different dengue serotype, facilitating virus entry into monocytes via Fc receptors, leading to increased viral replication (19, 20). While all DENV serotypes can lead to symptomatic or severe illness, variations in risk have been observed based on the serotype and infection status. Dengue illnesses associated with DENV-2 and DENV-4 are more commonly linked to secondary DENV infections, whereas DENV-1 and DENV-3 can often result in primary infections (9).
Regional specificity of the DENV serotypes has evolved over the years and global distribution of serotypes has gradually expanded. During the 1970s, all four serotypes were present in Southeast Asia, while only DEN-1 and DEN-2 were detected in Central America and Africa. By the 1990s, all DENV serotypes had been expanded globally, primarily as a result of expanding urban populations, increased vector density due to ineffective control programs, and the significant rise in commercial air travel facilitating (42).
From 2000-2002, all four serotypes were detected while DENV-3 was predominant in Bangladesh. DENV-1 and DENV-2 are predominant serotypes during 2013-2016. From 2013 to 2018, DENV-3 has not been reported. However, DENV-3 and DENV-4 were circulating in the neighboring country India so a secondary dengue outbreak was predicted (43). Since 2019, DENV-3 has been remerged as the predominant serotype (12). DENV-4 has been absent since 2013, however, this serotype was detected in 2022 (44) which could be responsible for severe secondary infection resulting in many dengue-related deaths in that year (33). In 2023, another serological shift has been observed as DENV-2 has become the predominant serotype this year. The shift in serotypes is considered to be a contributing factor to more severe infections and hospitalizations (12). DENV-4 has never been predominant in the last two decades of dengue outbreaks in Bangladesh, thus, it could potentially be responsible for the next severe dengue outbreak in the country (39).
PUBLIC HEALTH RESPONSE AND CHALLENGES: WHY DOES BANGLADESH KEEP FAILING TO MANAGE DENGUE?
The Directorate General of Health Services (DGHS) in Bangladesh has taken several actions to address the outbreak including coordination (e.g., establishment of a coordination committee for oversight and the formation of Dengue Control Rooms at various levels to collect epidemiological data), health system strengthening initiatives (e.g., repurposing hospitals for dengue case management, updating clinical management guidelines, and conducting capacity-building for healthcare professionals), risk communication (e.g., mass awareness campaigns, community engagement, and advocacy meetings), laboratory activities (e.g., dengue serotyping and distribution of diagnostic kits), and vector control activities (e.g., entomological survey, mosquito breeding site elimination and larvicidal and adult mosquito control) (12). Similar steps were also taken during previous large-scale outbreaks (39, 44).
Despite all the measures, Bangladesh continues to struggle to manage dengue outbreaks. Transparency International Bangladesh (TIB), the Bangladeshi branch of the Berlin-based Transparency International, highlighted several reasons for the high death rate this year, such as insufficient hospital manpower in comparison to patient numbers, delayed virus diagnosis, a lack of dengue prevention and control efforts, and inadequate medical facilities outside of Dhaka. TIB also included the lack of responsibility and accountability of the Government officials as a contributing factor to the failure of dengue management (45).
The extremely high number of dengue cases in recent years has overwhelmed the resource-limited healthcare system in Bangladesh (12). Insufficient access to intensive care unit (ICU) facilities at the district level and resource constraints for serological lab tests contribute to the challenges in managing severe dengue cases in Bangladesh (39).
The current surveillance system has been criticized for under-reporting dengue cases. The daily dengue bulletin provided by the DGHS relies on information from only 57 public and private hospitals in Dhaka, along with 81 hospitals at the district and divisional levels. However, there are approximately 16,000 healthcare facilities, including hospitals, clinics, diagnostic centers, and blood banks nationwide, offering dengue care. The inadequate information regarding the number of cases and circulating serotypes has been considered an obstacle to controlling dengue outbreaks (39, 46).
Since there is no approved vaccine available in Bangladesh and specific treatments are lacking, the primary approach to combat dengue is through vector control measures. However, these measures in Bangladesh have faced criticism for their ineffectiveness and are often regarded as stopgap measures (47, 48). Overreliance on chemical methods (larvicides and adulticides) rather than incorporating biological and physical methods has not been effective (45). Furthermore, insecticide resistance has made the existing chemical methods inefficient and wasteful. In a recent study, Ae. aegypti, the primary vector for dengue virus, exhibited extremely high levels of resistance to pyrethroids, a class of insecticides commonly used to target the mosquito (49). Moreover, efforts to prevent dengue are concentrated during the monsoon season rather than being sustained throughout the year. Bangladesh also lacks effective dengue cluster identification and innovative systems such as ovitrap surveillance to rapidly identify dengue-prone areas and trap female Aedes mosquitoes to prevent the spread of the outbreak (47).
Urbanization is known to be a significant contributing factor for creating the habitat for dengue vectors (1, 4, 13, 14) Rapid urbanization is now a common reality in Bangladesh, particularly in Dhaka. The number of multi-storey buildings and cars in Bangladesh has significantly increased since 2014 which is an important factor in the rise of dengue cases (46).
The dengue awareness program is insufficient in Bangladesh. A cross-sectional study with 1,010 respondents revealed that most people have heard about dengue but had misconceptions regarding mosquito breeding sites and their biting habits (50). Another recent study found that the knowledge, awareness, and preventive measures among slum dwellers in Dhaka city are inadequate, making them vulnerable to dengue infections (51). Therefore, the awareness program needs to be expanded and intensified to effectively educate the population about dengue prevention and control measures.
The ongoing political and financial crisis in Bangladesh has contributed to the worsening dengue situation by diverting attention from the dengue crisis. According to the former DGHS (Directorate General of Health Service) director Dr. ANM Nuruzzaman, the severity of dengue has been overlooked due to the country’s political turmoil (52). Lack of accountability, blame game, and ignoring outbreak warnings worsened the management situation (53). Public health experts have criticized the city corporation administration and local governments for their lack of sincerity in preventing the outbreak (54). It is crucial that political and administrative entities work collaboratively to ensure the well-being of the population and mitigate the impact of political, financial, and public health crises. Strengthening accountability mechanisms, and prioritizing public health issues is of profound importance to significantly enhance the preparedness and management of dengue outbreaks in Bangladesh. The government has a crucial role to play in managing this disease through evidence-based policies. This includes implementing mosquito surveillance and early warning systems, promoting source reduction through community engagement, and launching public education campaigns. Additionally, strengthening healthcare systems with trained professionals and proper resources is crucial. Collaboration with research institutions and international partners fosters innovation and knowledge sharing for better management of this persistent public health threat.
CONCLUSION
Since the first epidemic in 2000, dengue cases remained seasonal and often negligibly low until 2017. Over the past six years, a remarkably dangerous shift has occurred with more frequent and larger outbreaks, extending beyond traditional seasonal patterns. The increased rainfall and temperature due to climate change, as well as the periodic shifting of dengue serotypes, have been responsible for the severity of the dengue outbreak in recent years. The failure of the Government to implement an effective and adequate dengue management strategy has also been attributed to the worsening dengue crisis. In the face of changing climate, rapid unplanned urbanization, political unrest, financial crisis, and the recent dengue disaster, the nation stands on the brink of an impending catastrophe. It’s therefore crucially important to implement an effective strategy to combat dengue. Extensive serological, and entomological surveillance is of profound importance to predict and minimize the severity of dengue outbreaks. Adequate and proper vector control strategy remains essential to mitigate the ongoing public health crisis. As we navigate the dengue disaster in Bangladesh, it is incumbent upon policymakers, healthcare professionals, and communities alike to adopt a collaborative and proactive approach. Strengthening vector surveillance, enhancing diagnostic capabilities, and bolstering healthcare infrastructure is imperative for the early detection and management of outbreaks. What was once considered a seasonal nuisance has evolved into an unprecedented outbreak, underscoring systemic failures in epidemic management and response. Fostering community participation, promoting evidence-based interventions, and investing in sustainable vector control measures are essential for building resilience against future epidemics. In confronting the dengue crisis, Bangladesh stands at a crossroads, where the decisions we make today will shape the health and well-being of future generations.